Health Care Delivery for the Urban Poor: Reaching rural communities isn’t India’s only challenge
Editor’s note: This post was originally published at Searchlight South Asia. It is republished with permission.
Nearly one-third of India’s urban citizens live in crowded informal settlements or slum communities. UN-HABITAT has estimated that by the year 2020, India’s total slum population will cross 200 million people. City slums are characterized by poor access to clean water and adequate sanitation, the basic requirements for maintaining good hygiene and robust health. Health-wise, the urban poor are worse off than their middle- and high-income counterparts; they also appear to be worse off than their rural counterparts. Every year, Indian slums bear witness to how preventable illnesses cause thousands of deaths and millions of hours of forfeited productivity. The government is cognizant of the country’s urban health care challenges, but has thus far found it difficult to adequately serve the space.
Government Attitudes towards Urban Health Care
At an event organized by the Confederation of Indian Industry and the International Finance Corporation (IFC) in June 2012, Gajendra Haldea, Advisor to the Deputy Chairman of Infrastructure at the Indian Administrative Service (IAS), noted: “India is one of the largest countries in many sectors, but our health care is in shambles…In health care, the main challenge is not the initial capital expenditure. It is actually funding the recurring costs. The government has to step in to ensure that the recurring cost[s] can be subsidized or taken care of in some way.”
Despite the government’s indeterminate approach to recurring costs, its overall approach to health care has clearly evolved. In 1983, India’s National Health Policy adopted the Alma-Ata definition of primary health care to include “the provision of curative, preventive, promotive and rehabilitative health services.” This marked a shift in India’s attitude towards health care: previously, the focus had been on curative services; now, the stress was on integrated health services. As a result of this refocused approach to health care, India established 23,000 primary health care centers, 130,000 sub-centers and 150,000 health care institutions in rural areas.
In a statement to The Lancet about the general challenge with health care in India, Madabhushi Madan Gopal, Secretary of the Health and Family Welfare Department in the state of Karnataka, said: “The government lacks managerial skills and professionalism. We have also fallen behind in establishing community rapport and enabling convergence between the various departments that look at health, water and sanitation, etc.” Historically, Indian policy has been rural-centric. Though it is an imperfect system, the government has made considerable investment into a dedicated rural health care structure. But now, the country’s health care challenge has substantially grown to include the needs of urban health care. Because of shifting demographics caused by continuously increasing rural-to-urban migration, there needs to be a change in the Indian government’s lack of focus on urban health.
Though public health care services do exist in major cities, exploding urban populations mean that there are not enough primary health care facilities to cater to the public, nor have existing facilities been properly maintained. Health delivery for the urban poor is made even more difficult by their illegal and vulnerable status in cities. Most urban poor residents, then, are forced to consider private health care options, which are prohibitively – and, at times, dangerously – expensive. High out-of-pocket health-related expenditures are a key reason why many Indians fall further into poverty every year.
The National Family Survey
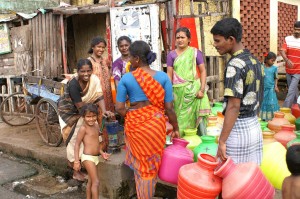 The intent of the Government of India cannot be questioned: it has adopted and implemented policy towards improving nationwide health care, but these efforts seem to lack efficacy. The scale of the challenge is huge and continues to grow, so it makes perfect sense that the government has taken steps to better understand the needs of the total population. In 1992, it launched the first National Family Health Survey. The International Institute for Population Sciences in Mumbai was selected as the official coordinator and guide for the Survey, and each iteration has been supported by various international organizations such as the Bill and Melinda Gates Foundation, the UK’s Department of International Development (DFID), different UN agencies and USAID. By investigating a representative sample of households across the country, the government has collected information on anemia, fertility, family planning, infant and child mortality, maternal and child health, and reproductive health and family planning services. The goal of this large nationwide survey is two-fold: to gather relevant data to inform policy and programs by the Ministry of Health and Family Welfare as well as other agencies, and to track emerging trends. The survey has been conducted three times: in 1991-1992, 1998-1999 and 2005-2006.
The intent of the Government of India cannot be questioned: it has adopted and implemented policy towards improving nationwide health care, but these efforts seem to lack efficacy. The scale of the challenge is huge and continues to grow, so it makes perfect sense that the government has taken steps to better understand the needs of the total population. In 1992, it launched the first National Family Health Survey. The International Institute for Population Sciences in Mumbai was selected as the official coordinator and guide for the Survey, and each iteration has been supported by various international organizations such as the Bill and Melinda Gates Foundation, the UK’s Department of International Development (DFID), different UN agencies and USAID. By investigating a representative sample of households across the country, the government has collected information on anemia, fertility, family planning, infant and child mortality, maternal and child health, and reproductive health and family planning services. The goal of this large nationwide survey is two-fold: to gather relevant data to inform policy and programs by the Ministry of Health and Family Welfare as well as other agencies, and to track emerging trends. The survey has been conducted three times: in 1991-1992, 1998-1999 and 2005-2006.
In the most recent survey, some alarming statistics regarding the health inequalities existing in India’s cities are reported. In his article “The state of urban health in India: comparing the poorest quartile to the rest of the urban population in selected states and cities,” Siddharth Agarwal, Executive Director of the Urban Health Resource Centre, points out an important fact about the latest survey results: “…A considerable proportion of the poorest population did not live in census slums…[This is] a reminder that programs to reduce urban poverty by addressing the needs of the poorest groups need to identify and focus on disadvantaged urban populations beyond [notified] slums.” An example of what Agarwal is talking about is how the 2005-2006 survey notes that there are a total of 967 slums in the smaller cities of Agra, Bally, Dehradun, Jamshedpur and Meerut. However, 413 of those slums are unlisted. Unlisted, or un-notified, slums are worse off because they suffer the consequences of no drainage, waterlogging and a lack of underground sewage systems — all of which give rise to preventable and possibly fatal health conditions. If the numbers of the urban poor cannot be accurately mapped, then how can the government – or any other agency – understand the breadth of the health care challenge India faces?
The Urban Health Resource Centre
As the latest survey and the 2011 Census demonstrate that there are more nuances to urban demographics than previously thought, the Indian government does need assistance in better serving urban areas, particularly in the face of the deteriorating health conditions of the urban poor. The Urban Health Resource Centre (UHRC), based in New Delhi, is a strong example of such assistance. It is an NGO addressing the “health, nutrition and wellbeing of the disadvantaged urban dwellers through demonstration programs, technical support to government and non-government sector, research, advocacy and knowledge dissemination through a consultative and partnership-based approach.” As the numbers of the urban poor multiply, the UHRC strongly believes that there is no better manager of public health care than the government. Its job as a non-governmental stakeholder, then, is to “provide technical support to make government policies and programs more pro-poor and inclusive and also strengthen the capacity of its city-level officers who manage the implementation of programs.” The UHRC has successfully worked with various stakeholders to design urban health programs across India.
An example of the interesting work the UHRC undertakes is the demonstration health programs it has launched in a few northern Indian cities. These projects are meant to improve the health of slum communities. City demonstration programs are the best way to enact proof of concept: by illustrating how different strategies can work in different settings, the UHRC is providing insights into what it takes to make urban health programs effective for the poor.
For instance, in Agra, the Government of India asked the UHRC to coordinate the development of a sample health proposal by the district health department and Municipal Corporation. The proposal is meant to guide the expansion of health services to Agra’s large urban poor population. In the proposal development process, it was found that approximately 50% of Agra’s population lives in slum communities – a statistic that is about five times greater than the 9.6% figure of the 2001 Census. After assessing listed and unlisted slums, the UHRC found that Agra had 393 slums, 183 of which were flagged as “the most vulnerable and in need of urgent attention.”
To propose a strategy, the UHRC consulted various government departments, municipal bodies and other non-governmental stakeholders. It was then concluded that a partnership between public agencies and more experienced NGOs would “be effective in rapidly expanding services to the large unreached sections of Agra city.” The partnership was formed between three NGOs – the Family Planning Association of India, Naujhil Integrated Rural Project for Health and Development and Shri Niroti Lal Buddhist Sansthan – and the State Government of Uttar Pradesh to provide health care to the underserved urban poor. The UHRC’s role is to provide technical support to the Uttar Pradesh government and NGOs in furthering the partnership initiative.
There are two partnership models being followed. The first model involves the launch of an urban health center (UHC) by an NGO in a previously unserved area by the government. These UHCs provide outpatient services, such as immunization, antenatal care and treatment of minor issues, as well as share health-related information and counseling. For this model to work, though, the UHRC and partner organizations knew that more health-related awareness needed to be spread within slum communities. To achieve this, the NGOs trained community link volunteers to share health information, counsel women in slums and mobilize the community to support health events (e.g. outreach camps). In each slum in Agra, women’s health groups were formed with 10-15 women each to support the activities of the partner NGOs. Under this first partnership approach, two new UHCs were set up and serve 107,000 people in 53 slums.
The second partnership model involves community mobilization and demand-generation activities by community link volunteers and the women’s groups. This approach is most appropriate in areas where government UHCs already exist. The UHRC facilitates links between slum communities and service providers, thereby promoting stronger health care demand and better utilization of existing services. Under this model, two of the partner NGOs have reached 100,000 urban poor people in 40 of Agra’s slums.
Emerging PPP Models
 The UHRC’s work is representative of how public-private partnerships (PPPs) in health care can work. And many experts in India believe that there is significant untapped potential in PPPs for health care. Of the PPP potential, Haldea from the IAS says: “Infrastructure projects were in shambles once. But they have come up recently because there’s a model framework in place and the government paid the attention that the sector demanded. We need to pick up lessons from infrastructure and see if [they] can be replicated in health care.”
The UHRC’s work is representative of how public-private partnerships (PPPs) in health care can work. And many experts in India believe that there is significant untapped potential in PPPs for health care. Of the PPP potential, Haldea from the IAS says: “Infrastructure projects were in shambles once. But they have come up recently because there’s a model framework in place and the government paid the attention that the sector demanded. We need to pick up lessons from infrastructure and see if [they] can be replicated in health care.”
The fact is that over the last two decades, health care PPP projects have emerged with varying results. Unsurprisingly, many of these projects have had a distinctly rural focus, but there are exceptions. For example, the Urban Slum Health Care Project in Andhra Pradesh is a partnership between the Ministry of Health and Family Welfare in Andhra Pradesh and local NGOs, who co-manage UHCs in Adilabad slums. Similar to the UHRC project in Agra, the objective of this particular PPP was to “increase the availability and utilization of health and family welfare services, to build an effective referral system, to implement national health programs and to increase health awareness and better health-seeking behavior among slum-dwellers.” In efforts to serve three million slum-dwellers, the PPP has set up 192 UHCs.
Most recently, the State Government of Uttar Pradesh is taking further steps to augment the efficacy of in-state health care PPPs. It organized a workshop in the state capital of Lucknow to formulate policy on implementing health care-related PPPs. The WHO and IFC made presentations on the different PPP models being employed across India and in 80 other countries. Dr. Shamit Sharma, Managing Director of the Rajasthan Medical Services Corporation, was in attendance and said that, “It’s difficult but quite possible to implement PPP.”
Conclusion
In a country as large as India, it is undeniable that the government has a huge role to play as purveyor and facilitator of health care services, but it is not the only stakeholder that can make a difference. Renowned cardiac surgeon and founder of the Narayana Hrudayalaya hospital in Karnataka, Dr. Devi Shetty, says: “I believe that primary health care must be offered free, but it is not mandatory for the government to do this. Governments across the world have failed in providing free primary health care to the community. Private players can provide better services as they operate to economies of scale, and bring in professionalism. If health insurance becomes mandatory, primary health services offered by the private sector will translate into benefits for the poor.”
As rural health care models proliferate and are refined in India, it also becomes obvious that the needs of urban health care are becoming more relevant and immediate. There are significant costs – economic and health — to the conditions borne by the urban poor, and different models are needed to alleviate and promote the poor’s primary health care needs. There is no magic formula to health care delivery, but there does seem to be a growing climate of experimentation in reaction to an ill-equipped urban health care system. The private sector, in conjunction with the massive networks of the government, can be what tips the balance for the better and changes the urban health care story across the country.
- Categories
- Health Care
- Tags
- governance, public health
